Immune responses to infectious microbes vary among individuals within a population, and between different populations—a result of selective pressures from environmental and genetic factors, as well as from the infectious microbes themselves. Now, results from a new study show—for the first time—marked differences in the immune response to infectious microbes between Americans of African descent and Americans of European descent. These differences are mostly genetic—inherited from our ancestors and influenced by relatively recent natural selection.
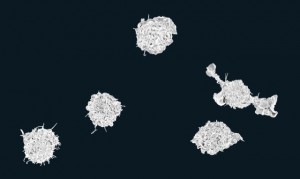
The study (Genetic Ancestry and Natural Selection Drive Population Differences in Immune Responses to Pathogens), published in the journal Cell on October 20, 2016, was carried out in a human population consisting of 175 American individuals, 80 of African descent, and 95 of European descent. The 175 participants provided blood samples. The researchers used the blood samples to obtain macrophages—a type of white blood cell that wears many hats during the immune response. One of the macrophages’ functions is to participate in the innate immune response by sensing the presence of infectious microbes, and keeping these microbes under control while initiating the inflammatory response. During the inflammatory response, macrophages directly kill the invading microbes through a process called phagocytosis. In addition, they release chemical messengers that call other white blood cells to help resolve the infection, while moving the immune response to the next stage—the adaptive immunity stage.
The researchers infected the macrophages with live bacteria, either Listeria monocytogenes (a Gram-positive bacterium) or Salmonella typhimurium (a Gram-negative bacterium). These intracellular bacterial species specifically infect macrophages and, if the immune response is not strong enough, are able to grow and multiply within them. The researchers found markedly stronger response to infection induced in macrophages from individuals of African descent. Indeed, African ancestry specifically predicted a stronger inflammatory response and reduced intracellular bacterial growth. This effect was particularly noticeable when macrophages were infected with Listeria. There were no significant difference in the initial number of bacteria infecting macrophages. However, 24 hours after infection, the number of bacteria inside the macrophages from individuals with high levels of African ancestry was 3.2-fold lower than that of macrophages from individuals of European ancestry. The study results also show that these differences are under genetic control.
Luis Barreiro, senior author of the study, said in a press release: “Although we found these differences in immune responses between African and European Americans, we are still unable to demonstrate what evolutionary pressures led to the observed differences. One of our hypotheses is that in the prehistoric period, after human populations had migrated out of Africa, they were exposed to fewer pathogens (bacteria, viruses, parasites), which reduced the immune response and thus tissue inflammation. This reduction in the immune response (and inflammation) was most likely an advantage because of the adverse consequences of acute or chronic inflammation, which are major contributors to the development of autoimmune inflammatory diseases.”
Indeed, while short-term inflammation is necessary to eliminate invading microbes, long-term inflammation may lead to the development of chronic inflammatory disorders, as for example cardiovascular disease, or certain autoimmune diseases.
Barreiro added: “The immune system of African Americans responds differently, but we cannot conclude that it is better, since a stronger immune response also has negative effects, including greater susceptibility to autoimmune inflammatory diseases such as Crohn’s disease. Too much inflammation can damage organs and leave sequelae. In short, a strong immune response can be beneficial in some areas but a disadvantage in others.”



In this article, studies were conducted on blood samples of 175 Americans. Of those Americans, 80 were African American and 95 were Americans of European descent. The results showed a difference in macrophage activity in both ethnicities. Ultimately though, it was not concluded that either ethnicity acquired the better evolutionary change. I found this article to be absolutely fascinating. To think that we, as people of varying backgrounds, have existed long enough and in such diverse environments that we have developed differences genomically is almost hard to believe. In fact, I couldn’t believe it. So, I discovered an article that actually stated that permanent evolutionary changes take about one million years to come into effect (1)! It also stated that “rapid changes in local populations often don’t continue,” and when considering the world, North America is a local population. Therefore, it may be too soon to jump to conclusions about the current genomic modification in macrophages and treat them as evolved traits.
Citation:
Uyeda J, Hansen T, Arnold S, Pienaar J. The million-year wait for macroevolutionary bursts. Proceedings of the National Academy of Sciences of the United States of America [serial online]. 2011:15908. Available from: JSTOR Journals, Ipswich, MA. Accessed November 13, 2016.
I think you are strongly underestimating the impact of how small changes in the genome can make a large impact in the workings of the body. For instance, science has shown that at some point our European ancestors began to merge with portions of the Neanderthal population, as evidenced through fossil records. While Neanderthals became extinct around 40,000 years ago they too seem to have had an impact upon our genome. A 2016 study in Cell (Quach et al., http://dx.doi.org/10.1016/j.cell.2016.09.024) gives us insight into how much this interbreeding with a human subspecies permanently effected the population. The study collected 200 samples from people living in Belgium, with half the samples from those of African decent and half from European decent. Similarly to the study described in this post, there was a marked difference in the immune systems of the two populations, with the African samples having a stronger anti-viral and more pronounced inflammatory response. The results showed that the introduction of Neanderthal DNA into the European population caused regulatory changes within the immune response, dampening the overall effect. This highlights the various ways that natural selection can change our genome and overall functioning, both through environment and introduction of new genetic material into the population. However, it can occur over a much shorter time period than millions of years.
Quentin,
Like Ashley, I disagree with your scepticism regarding the rapid evolutionary mechanism acting on populations. With that said, I am with you in fascination. I am most interested in projecting these findings into the future. Specifically, the role theses genetic differences play on treatment of inflammatory disease for patients of diverse backgrounds. The dream would be to have tailored therapies for patients based on their unique genetic profile.